Have you ever noticed persistent dark spots on your lower leg and wondered what they are or how to get rid of them You’re not alone. Many people experience various forms of skin discoloration on their legs, ranging from small, faint marks to more prominent patches. These spots, often a source of cosmetic concern, can sometimes indicate underlying skin conditions or simply be the result of everyday wear and tear on our skin.
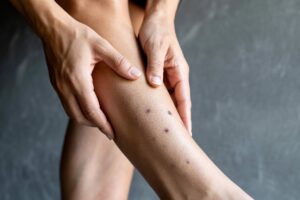
Our legs, frequently exposed to the elements and prone to minor injuries, are particularly susceptible to developing hyperpigmentation. Understanding the different types of lower leg dark spots and their root causes is the first step toward effective management. Whether it’s post-inflammatory hyperpigmentation from an old bug bite, sun spots from years of sun exposure, or something else entirely, knowing what you’re dealing with can guide you to the right solutions.
In this comprehensive guide, we’ll delve deep into the world of dark spots on lower leg. We’ll explore their common causes, discuss when it’s time to consult a doctor, and provide you with practical advice on both treating existing pigmentation and preventing new spots from forming. Get ready to uncover the secrets to achieving clearer, more even-toned skin on your lower legs!
What Are Dark Spots on Lower Legs?
Dark spots on lower leg are essentially areas of skin that have become darker than the surrounding skin. This darkening, known as hyperpigmentation, occurs when there’s an excess production of melanin, the pigment responsible for skin, hair, and eye color. These spots can vary in size, shape, and color, appearing as light brown, dark brown, or even reddish-brown patches.
While often benign, these spots can be a nuisance. They are not typically painful or itchy, but their presence can affect one’s self-confidence, especially when wearing shorts or skirts. The specific appearance and cause of lower leg dark spots can differ significantly, leading to various types of hyperpigmentation:
- Post-Inflammatory Hyperpigmentation (PIH): This is one of the most common types of dark pigmentation on legs. It occurs after an injury or inflammation, such as a cut, burn, bug bite, acne, eczema flare-up, or even an ingrown hair. As the skin heals, it produces too much melanin, leaving behind a dark mark.
- Sun Spots (Solar Lentigines): Also known as age spots or liver spots, these flat, brown or black spots are caused by prolonged sun exposure over time. They are most common on areas frequently exposed to the sun, including the lower legs.
- Venous Stasis Dermatitis: This condition results from poor circulation in the leg veins (venous insufficiency), leading to blood pooling and pressure. Over time, this can cause reddish-brown or dark brown discoloration, often around the ankles and shins, accompanied by swelling, itching, and sometimes skin thickening.
- Drug-Induced Pigmentation: Certain medications can cause skin darkening as a side effect.
- Melasma: While more common on the face, melasma can occasionally appear on other body parts, including the legs. It’s characterized by symmetrical, splotchy brown or gray-brown patches, often triggered by hormonal changes (e.g., pregnancy, birth control) and sun exposure.
- Freckles: Small, flat brown spots that often appear in clusters, especially after sun exposure. While common, they are typically genetic and less often a concern for “dark spots” unless they are large or changing.
Common Causes of Dark Spots on Lower Legs
Understanding the triggers behind dark spots on lower leg is crucial for both treatment and prevention. Here are the primary culprits:
Sun Exposure
The sun’s ultraviolet (UV) rays are a major contributor to hyperpigmentation on legs. Unprotected exposure stimulates melanin production as a protective mechanism, leading to the formation of sun spots (solar lentigines) and worsening existing pigmentation. Even incidental sun exposure, like walking outdoors or driving, can accumulate over time.
Post-Inflammatory Hyperpigmentation (PIH)
As mentioned, PIH is a leading cause of dark spots on shins and calves. Any inflammatory event or injury can trigger it. Common examples include:
- Bug Bites: Mosquito bites, spider bites, or other insect stings often leave behind a dark mark after they heal, especially if scratched.
- Cuts, Scrapes, and Abrasions: Minor injuries are common on the legs and can lead to lasting discoloration.
- Eczema and Psoriasis: Chronic inflammatory skin conditions can cause significant PIH, particularly in individuals with darker skin tones.
- Folliculitis and Ingrown Hairs: Inflammation around hair follicles, often from shaving or waxing, can result in persistent dark spots.
- Burns: Even minor burns can leave behind significant post-inflammatory hyperpigmentation.
Venous Insufficiency and Stasis Dermatitis
For many, particularly older adults, brown spots on lower legs can be a sign of underlying circulatory issues. Venous insufficiency occurs when the valves in the leg veins don’t function properly, allowing blood to pool. This increased pressure can lead to fluid leakage and inflammation, eventually causing hemosiderin staining (iron deposits from red blood cells) which manifests as a reddish-brown or dark brown discoloration, often around the ankles and lower calves. This condition is called stasis dermatitis.
Drug-Induced Pigmentation
Certain medications can cause hyperpigmentation as a side effect. These can include some antibiotics, anti-malarial drugs, anti-inflammatory drugs, and even some chemotherapy agents. If you’ve started a new medication and notice new dark pigmentation on legs, consult your doctor.
Melasma
Though less common on the legs than on the face, melasma can sometimes appear on the body. It’s characterized by patchy, symmetrical dark areas and is often linked to hormonal fluctuations (pregnancy, birth control) combined with sun exposure. It can be particularly stubborn to treat.
Age Spots / Lentigines
These are essentially sun spots that become more prevalent with age due to cumulative sun exposure over a lifetime. They are flat, oval-shaped brown spots that appear on sun-exposed areas, including the lower legs.
When to See a Doctor
While most dark spots on lower leg are benign, it’s always wise to have any new or changing skin lesion checked by a healthcare professional, especially a dermatologist. You should seek medical advice if a dark spot:
- Is new, rapidly growing, or changing in size, shape, or color.
- Has irregular borders or multiple colors.
- Is itchy, bleeding, or painful.
- Appears suddenly without any apparent cause.
- Is accompanied by other symptoms like swelling, redness, warmth, or pain in the legs, which could indicate venous issues or infection.
A doctor can accurately diagnose the type of dark spot and rule out more serious conditions like melanoma or other skin cancers.
Effective Strategies to Treat Dark Spots on Lower Legs
Treating dark spots on lower leg requires patience and a consistent approach. The best strategy often involves a combination of methods, tailored to the specific cause and type of hyperpigmentation.
Topical Treatments
Over-the-counter (OTC) and prescription topical creams can be highly effective in fading hyperpigmentation on legs by inhibiting melanin production or promoting skin cell turnover.
- Hydroquinone: Often considered the gold standard for hyperpigmentation, hydroquinone works by decreasing the production of melanin. Available OTC in lower concentrations (2%) and by prescription in higher strengths (4% or more). Use under dermatologist supervision due to potential side effects with prolonged use.
- Retinoids (Retinol, Tretinoin): These Vitamin A derivatives accelerate cell turnover, helping to shed pigmented skin cells and bring new, unpigmented cells to the surface. Retinol is OTC, while tretinoin is prescription-strength.
- Vitamin C: A potent antioxidant that brightens skin, inhibits melanin production, and protects against sun damage. Look for serums with L-ascorbic acid.
- Niacinamide (Vitamin B3): Reduces melanin transfer to skin cells and has anti-inflammatory properties, making it excellent for PIH.
- Alpha Arbutin/Kojic Acid: Natural alternatives to hydroquinone that also inhibit melanin production.
- Azelaic Acid: Effective for PIH and melasma, it reduces inflammation and inhibits tyrosinase (an enzyme essential for melanin production).
- Alpha Hydroxy Acids (AHAs) & Beta Hydroxy Acids (BHAs): Glycolic acid (AHA) and salicylic acid (BHA) are chemical exfoliants that help remove the top layer of pigmented skin cells, revealing brighter skin underneath. They are often found in lotions and body washes.
Professional Procedures
For more stubborn or widespread lower leg dark spots, professional treatments offered by dermatologists can provide more dramatic results.
- Laser Therapy: Various lasers (e.g., Q-switched, picosecond, fractional lasers) can specifically target and break down melanin deposits without damaging surrounding skin. This is highly effective for sun spots and some forms of PIH.
- Chemical Peels: A dermatologist applies a chemical solution to the skin, causing it to exfoliate and eventually peel off, revealing new, less pigmented skin. Different strengths are available.
- Microdermabrasion: A minimally invasive procedure that uses a special applicator to gently “sand” away the thick outer layer of skin, improving tone and texture.
- Cryotherapy: For individual, well-defined dark spots, liquid nitrogen can be used to freeze and destroy the pigmented cells.
Natural Remedies
While often less potent than medical treatments, some natural remedies may offer mild benefits for dark spots on lower leg, particularly for recent or faint marks. Always patch test before widespread use.
- Aloe Vera: Known for its skin-healing and soothing properties, it may help in the fading process over time.
- Lemon Juice: Contains natural bleaching properties due to its Vitamin C content. However, it can be irritating and increase sun sensitivity, so use with extreme caution and never before sun exposure.
- Turmeric: A common ingredient in traditional medicine, turmeric contains curcumin, which may inhibit melanin production. Be aware that it can temporarily stain skin yellow.
Preventing Dark Spots on Lower Legs
Prevention is always better than cure, especially when it comes to dark spots on lower leg. By adopting a few key habits, you can significantly reduce your risk of developing new spots and worsening existing ones.
Sun Protection
This is arguably the most crucial step. Protecting your legs from UV radiation will prevent new sun spots and stop existing dark spots from getting darker.
- Apply Sunscreen Daily: Use a broad-spectrum sunscreen with an SPF of 30 or higher on your lower legs every day, even on cloudy days or when you’ll be indoors near windows. Reapply every two hours when outdoors.
- Wear Protective Clothing: Opt for long pants or skirts, or UPF (Ultraviolet Protection Factor) clothing when spending extended time outdoors.
- Seek Shade: Limit your time in direct sunlight, especially during peak hours (10 AM to 4 PM).
Managing Skin Conditions
If you suffer from conditions like eczema or psoriasis, diligent management can prevent the inflammation that leads to PIH.
- Follow Treatment Plans: Adhere to your dermatologist’s recommendations for managing flares.
- Moisturize Regularly: Keeping skin hydrated can reduce irritation and strengthen the skin barrier.
- Avoid Scratching: Resist the urge to scratch itchy areas, as this worsens inflammation and increases the likelihood of dark spots.
Avoiding Injury
Minimize cuts, scrapes, and bug bites that can lead to PIH.
- Be Careful During Activities: Wear appropriate clothing (e.g., long pants when gardening or hiking) to prevent scrapes.
- Use Insect Repellent: Protect yourself from bug bites, especially in mosquito-prone areas.
- Shave Gently: Use a sharp razor, shaving cream, and shave in the direction of hair growth to prevent irritation and ingrown hairs. Consider alternatives like epilation or laser hair removal if shaving frequently causes issues.
Proper Leg Care
- Gentle Exfoliation: Regular, gentle exfoliation (e.g., with an AHA/BHA body wash or lotion) can help keep skin smooth and prevent dead skin cell buildup that can make dark spots appear worse.
- Moisturize Consistently: Hydrated skin heals better and looks healthier. Choose a fragrance-free moisturizer, especially if you have sensitive skin.
- Address Venous Issues: If you suspect venous insufficiency, consult a doctor. Compression stockings and elevating your legs can help manage symptoms and prevent further discoloration.
Recommended Products
La Roche-Posay Anthelios Melt-in Milk Sunscreen SPF 60
A broad-spectrum, water-resistant sunscreen ideal for daily body protection, crucial for preventing and managing dark spots.
CeraVe Daily Moisturizing Lotion
A gentle, fragrance-free moisturizer with ceramides and hyaluronic acid to hydrate and restore the skin’s protective barrier, aiding in skin health and healing.
TruSkin Vitamin C Serum for Face
A popular Vitamin C serum that can be used on the body for its antioxidant and brightening properties, helping to fade dark spots and even skin tone.
AmLactin Daily Moisturizing Lotion
Contains lactic acid (an AHA) for gentle exfoliation and intense moisturization, helping to smooth rough skin and improve the appearance of dark spots.
FAQ Section
Q1: Are dark spots on lower legs normal?
Yes, dark spots on lower leg are quite common and often normal. They can result from everyday occurrences like sun exposure, healing from minor injuries (bug bites, cuts), or inflammatory skin conditions such as eczema. While frequently benign, it’s important to monitor them and consult a doctor if they change in appearance or cause concern.
Q2: How long does it take for dark spots on legs to fade?
The fading time for lower leg dark spots varies greatly depending on their cause, depth, and the treatment approach. Post-inflammatory hyperpigmentation can take several months to a year or more to fade naturally. Sun spots might be more persistent. With consistent use of topical treatments and diligent sun protection, you might start seeing improvements in a few weeks, but significant fading often requires 3-6 months or longer. Professional treatments can accelerate the process.
Q3: Can diet help with dark spots on lower legs?
While diet alone cannot directly eliminate dark pigmentation on legs, a healthy, antioxidant-rich diet can support overall skin health and healing. Foods rich in Vitamin C and E, for example, can help protect skin cells from damage and aid in the repair process. Staying hydrated is also crucial for healthy skin. However, dietary changes are generally complementary to, not a replacement for, topical treatments and sun protection.
Q4: Is sun exposure the main cause of dark spots on lower legs?
Sun exposure is a very significant cause, particularly for solar lentigines (sun spots) and for worsening existing dark spots on lower leg from other causes like PIH. UV radiation stimulates melanin production, making any hyperpigmented area darker and harder to fade. However, it’s not the *only* cause; post-inflammatory hyperpigmentation, venous insufficiency, and even certain medications are also common culprits.
Q5: When should I worry about a dark spot on my leg?
You should be concerned about a dark spot on your lower leg if it exhibits any of the “ABCDEs” of melanoma: Asymmetry, irregular Border, varied Color, a Diameter larger than 6mm, or Evolving (changing) in size, shape, or color. Other red flags include itching, bleeding, or pain. If you notice any of these changes, or if a spot appears suddenly and grows rapidly, consult a dermatologist immediately to rule out skin cancer.
Conclusion
Dealing with dark spots on lower leg can be a frustrating experience, but with the right knowledge and consistent effort, achieving clearer, more even-toned skin is absolutely possible. We’ve explored that these spots are often a result of sun exposure, post-inflammatory hyperpigmentation from injuries or skin conditions, or even underlying circulatory issues like venous stasis dermatitis.
The key takeaways are clear: sun protection is paramount, both for preventing new spots and keeping existing ones from worsening. Combining diligent sunscreen use with targeted topical treatments like retinoids, Vitamin C, or hydroquinone can significantly accelerate fading. For more stubborn cases, professional dermatological procedures offer effective solutions.
Remember, patience is a virtue when treating hyperpigmentation. Skin cell turnover takes time, and results won’t appear overnight. If you’re ever unsure about the nature of a dark spot or if it changes, don’t hesitate to consult a dermatologist. They can provide an accurate diagnosis and tailor a treatment plan specifically for your needs. Embrace a consistent skincare routine and enjoy the journey to healthier, more radiant skin on your lower legs!
“`
