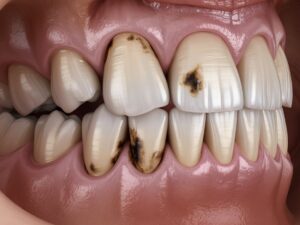
Discovering a dark spot on your tooth can send a ripple of anxiety through anyone. Immediately, the question often arises: Are dark spots on teeth cavities? It’s a natural concern, as cavities are a common dental problem that can manifest as dark discoloration. However, the truth is more nuanced. While some dark spots indeed signal tooth decay, many others are harmless stains or other benign issues. Understanding the difference is crucial for your dental health and peace of mind.
In this comprehensive guide, we’ll delve deep into the various reasons behind tooth discoloration. We’ll explore when a dark spot might genuinely be a cavity and when it’s simply an aesthetic concern. From common dietary stains to the more serious signs of decay, we’ll equip you with the knowledge to better understand what you’re seeing. More importantly, we’ll emphasize the irreplaceable role of your dentist in accurate diagnosis and effective treatment. So, if you’ve been pondering, “Are dark spots on teeth cavities?”, read on to uncover the answers and learn how to maintain a bright, healthy smile.
Understanding Dark Spots on Teeth: More Than Just Cavities
The Immediate Concern: Are Dark Spots On Teeth Cavities?
When you spot a dark mark on your tooth, it’s perfectly normal for your mind to jump to the worst-case scenario: a cavity. And sometimes, you might be right. Dental cavities, also known as tooth decay or caries, often appear as brown, black, or grey spots or holes on the tooth surface. These spots are the result of acids produced by bacteria eroding the tooth enamel and dentin. If left untreated, they can grow larger, cause pain, infection, and eventually lead to tooth loss.
However, it’s vital to understand that not every dark spot signifies a cavity. The mouth is a complex environment, and various factors can contribute to tooth discoloration. Rushing to self-diagnose can lead to unnecessary worry or, conversely, a false sense of security. The first and most important step upon noticing any persistent dark spot is to schedule an appointment with your dentist for a professional evaluation.
Common Causes of Dark Spots That Aren’t Cavities
Many dark spots on teeth are merely surface stains or other non-carious issues. Here are some of the most common culprits:
- Extrinsic Stains: These are surface stains that accumulate on the enamel from external sources.
- Food and Drink: Coffee, tea, red wine, dark sodas, berries, and soy sauce are notorious for staining teeth.
- Tobacco: Smoking or chewing tobacco can cause significant yellow, brown, or black stains.
- Certain Medications: Some liquid iron supplements or chlorhexidine mouthwashes can cause temporary dark staining.
- Tartar (Calculus) Buildup: When plaque hardens, it forms calculus, or tartar. This substance can be yellow, brown, or even black, especially along the gum line or between teeth, mimicking a dark spot. Poor oral hygiene allows plaque to accumulate and calcify.
- Intrinsic Stains: These stains are incorporated into the tooth structure itself.
- Tetracycline Stains: If a child is exposed to tetracycline antibiotics during tooth development, their permanent teeth can develop dark grey or brown bands.
- Fluorosis: Excessive fluoride intake during tooth formation can lead to white, brown, or black spots on the enamel.
- Trauma: An injury to a tooth can cause the nerve to die, leading to internal discoloration that makes the tooth appear darker.
- Aging: As we age, the outer enamel layer thins, revealing more of the naturally yellowish dentin beneath, which can sometimes appear darker.
- Amalgam Fillings: Old silver-colored (amalgam) fillings can sometimes make the surrounding tooth structure appear darker or even cause a greyish hue due to metallic ions leaching into the dentin over time.
- Developmental Anomalies: In some cases, teeth can develop with areas of hypomineralization or other structural irregularities that appear as dark spots.
When Dark Spots Are Cavities: Recognizing the Signs
While a dentist is the only one who can definitively confirm a cavity, there are some indicators that suggest a dark spot might indeed be tooth decay:
- Location: Cavities often form in specific areas:
- Pits and Fissures: The chewing surfaces of molars and premolars have grooves where food particles and bacteria can easily get trapped.
- Between Teeth: Decay can occur where teeth touch, often hidden from view and requiring X-rays to detect.
- Along the Gum Line: Receding gums can expose softer root surfaces, which are more susceptible to decay.
- Texture: Unlike smooth stains, a cavity might feel rough, sticky, or soft when probed gently (though you should avoid probing aggressively yourself). A dental explorer will stick to decayed enamel.
- Color Progression: Early decay often appears as a white spot, indicating demineralization. Over time, as bacteria continue to break down the tooth structure and absorb pigments, this spot can turn light brown, then dark brown, and eventually black.
- Associated Symptoms: As a cavity progresses, you might experience:
- Sensitivity: To hot, cold, or sweet foods and drinks.
- Pain: A toothache, ranging from mild to sharp pain, especially when biting down.
- Visible Holes or Pits: In advanced stages, a noticeable hole or pit may be present.
- Bad Breath or Unpleasant Taste: Due to bacterial activity.
The Role of Dental Professionals in Diagnosis
Given the variety of causes, a professional diagnosis is paramount. Dentists use several tools and techniques to determine if a dark spot on your tooth is a cavity or something else:
- Visual Examination: They will carefully examine your teeth, looking for discoloration, pits, and fissures.
- Dental Explorer: A small, sharp instrument used to gently probe the tooth surface. If it catches or sticks, it often indicates a soft, decayed area.
- Dental X-rays: Bitewing X-rays are crucial for detecting decay between teeth or under existing fillings, areas not visible during a visual exam.
- Transillumination: Shining a bright light through the tooth can reveal shadows that indicate decay.
- Dye Stains: Sometimes, a special dye is applied that highlights decayed areas.
Early detection is key, whether it’s identifying a cavity that needs a filling or a stain that can be easily removed. Ignoring any dark spots can lead to more extensive and costly treatments down the line.
Differentiating Between Stains and Cavities
Key Indicators to Look For
While only a dentist can give a definitive diagnosis, understanding these distinctions can help you better describe your symptoms and concerns:
- Smooth vs. Rough Texture: Stains are typically smooth to the touch, though sometimes they might be slightly rough due to tartar buildup. Cavities, especially advanced ones, often feel rough, soft, or sticky when gently probed.
- Location: Stains can appear anywhere on the tooth, often along the gum line, in pits, or on broad surfaces. Cavities, however, have a higher predilection for specific areas like deep grooves, between teeth, or at the gum line.
- Associated Symptoms: Stains typically don’t cause pain or sensitivity. Cavities, on the other hand, often do, especially as they progress, leading to discomfort with hot, cold, or sweet foods.
- Color Change Over Time: While stains can darken over time with continued exposure, cavities often start as a white spot (demineralization) and then gradually darken as decay progresses.
Self-Assessment vs. Professional Diagnosis
It’s important to differentiate what you can observe at home from what requires a professional eye. You can certainly notice a dark spot, its location, and whether it causes any pain or sensitivity. However, you cannot accurately assess the depth of the spot, its texture (without risking damage), or whether it’s truly decay or a stain. Over-the-counter whitening products, for example, might lighten surface stains but will do nothing for a cavity, allowing it to worsen undetected. Therefore, any persistent or concerning dark spot warrants a visit to your dentist.
Treatment Options for Dark Spots on Teeth
Treating Stains
If your dark spots are determined to be stains, there are several effective treatment options:
- Professional Dental Cleaning: A hygienist can remove most extrinsic stains and tartar buildup using specialized tools. This is often the first line of defense and can significantly brighten your smile.
- Whitening Toothpastes: These contain mild abrasives or chemical agents that help polish away surface stains. They are effective for minor staining but won’t change the intrinsic color of the tooth.
- At-Home Whitening Kits: These typically involve trays or strips with peroxide-based bleaching agents. They can be effective for moderate staining but should be used with caution and preferably after consulting your dentist.
- Professional Teeth Whitening (Bleaching): Performed in a dental office, this uses stronger bleaching agents and often light or laser activation for faster, more dramatic results.
- Cosmetic Bonding or Veneers: For intrinsic stains (like tetracycline stains or severe fluorosis) that don’t respond to whitening, bonding (applying tooth-colored resin) or veneers (thin shells covering the tooth surface) can mask the discoloration.
Treating Cavities
If the dark spot is confirmed to be a cavity, treatment aims to remove the decayed portion and restore the tooth’s structure and function:
- Fillings: For small to moderate cavities, the decayed material is removed, and the tooth is filled with a restorative material. Common options include composite resin (tooth-colored), amalgam (silver), or glass ionomer.
- Crowns: If the decay is extensive and has weakened a significant portion of the tooth, a crown (a cap covering the entire tooth) may be necessary to protect and restore it.
- Root Canal Therapy: If the decay reaches the pulp (the innermost part of the tooth containing nerves and blood vessels), causing infection, a root canal may be performed. This involves removing the infected pulp, cleaning the root canals, and sealing them. A crown usually follows a root canal.
- Extraction: In severe cases where the tooth is too damaged to be saved, extraction (removal) may be the only option. The missing tooth can then be replaced with an implant, bridge, or partial denture.
Addressing Other Causes
- Amalgam Filling Replacement: If an old amalgam filling is causing aesthetic concerns or structural issues, it can be replaced with a tooth-colored composite filling or a crown.
- Trauma-Induced Discoloration: If a tooth darkens due to trauma, it may indicate nerve damage. Root canal therapy might be needed if the nerve dies. Cosmetic solutions like internal bleaching or veneers can address the discoloration.
Preventing Dark Spots and Cavities
Prevention is always better than cure, especially when it comes to dental health. By adopting good habits, you can significantly reduce your risk of both stains and cavities.
Oral Hygiene Best Practices
- Brush Twice Daily: Use a fluoride toothpaste and brush for at least two minutes, paying attention to all surfaces of your teeth. An electric toothbrush can be particularly effective at removing plaque and surface stains.
- Floss Daily: Flossing removes food particles and plaque from between your teeth and under the gum line, areas your toothbrush can’t reach. This is critical for preventing interproximal cavities and gum disease.
- Use Mouthwash: An antiseptic or fluoride mouthwash can help reduce bacteria and strengthen enamel, offering an extra layer of protection.
- Tongue Cleaning: Brushing or scraping your tongue can remove bacteria that contribute to bad breath and plaque formation.
Dietary Considerations
- Limit Staining Foods and Drinks: Reduce consumption of coffee, tea, red wine, dark sodas, and highly pigmented foods. If you do consume them, consider rinsing your mouth with water afterward or drinking through a straw to minimize contact with teeth.
- Reduce Sugary and Acidic Foods: Sugary foods and drinks feed the bacteria that produce cavity-causing acids. Acidic foods (like citrus fruits and sodas) can erode enamel, making teeth more susceptible to both stains and decay.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and bacteria, and stimulates saliva production, which naturally cleanses and remineralizes teeth.
Regular Dental Check-ups and Cleanings
Visiting your dentist every six months for a professional cleaning and check-up is non-negotiable. These appointments allow your hygienist to remove plaque and tartar buildup that you might miss, and your dentist to identify early signs of cavities, gum disease, or other issues before they become serious problems. They can also address any dark spots you’ve noticed and determine if dark spots on teeth are cavities or just stains.
Protective Measures
- Dental Sealants: For children and adults, sealants can be applied to the chewing surfaces of molars and premolars to fill in deep grooves, creating a smooth surface that’s easier to clean and less prone to decay.
- Fluoride Treatments: Your dentist may recommend professional fluoride treatments, especially if you’re at high risk for cavities, to strengthen your enamel.
Recommended Products
An electric toothbrush can provide superior plaque removal compared to a manual brush, helping prevent stains and cavities more effectively.
Fluoride Toothpaste
A toothpaste with fluoride helps strengthen tooth enamel and protect against acid attacks, reducing the risk of cavities.
High-Quality Dental Floss
Regular flossing is essential for removing plaque and food particles from between teeth, preventing cavities and gum disease in hard-to-reach areas.
Antiseptic Mouthwash
Using an antiseptic mouthwash can help reduce bacteria in your mouth, contributing to fresher breath and a healthier oral environment.
FAQ Section
Q1: Can dark spots on teeth go away naturally?
A: Most dark spots on teeth, whether they are stains or cavities, do not go away naturally. Surface stains can sometimes be minimized with improved oral hygiene, but professional cleaning or whitening is usually required for significant removal. Cavities, by definition, are areas of tooth decay that require dental intervention to stop their progression and restore the tooth. Ignoring them will only allow them to worsen.
Q2: What’s the difference between a dark spot and a black spot on a tooth?
A: The terms “dark spot” and “black spot” are often used interchangeably to describe tooth discoloration. A black spot simply indicates a darker degree of discoloration, which could be a very deep stain (e.g., from tobacco or specific medications) or a more advanced cavity. Generally, the darker the spot, the more urgent it is to have it checked by a dentist, as black often signals significant decay or heavy staining.
Q3: Are dark spots on wisdom teeth always cavities?
A: Not necessarily. Like any other tooth, wisdom teeth can develop dark spots due to stains or cavities. However, wisdom teeth are often harder to clean due to their position at the very back of the mouth, making them more susceptible to plaque buildup and decay. If a dark spot appears on a wisdom tooth, it’s particularly important to get it checked, as it might indicate a cavity that needs immediate attention.
Q4: How do dentists tell if a dark spot is a cavity?
A: Dentists use a combination of methods. They perform a thorough visual examination, often using a dental explorer to gently probe the spot to check for softness or stickiness indicative of decay. Dental X-rays are crucial for detecting cavities between teeth or under existing fillings, which are not visible to the naked eye. Sometimes, specialized dyes or transillumination (shining a light through the tooth) may also be used to aid in diagnosis.
Q5: Can I whiten away dark spots that are cavities?
A: No, you cannot whiten away dark spots that are cavities. Whitening treatments work by bleaching the tooth enamel to remove stains and lighten the overall tooth shade. They do not remove or treat tooth decay. If a dark spot is a cavity, whitening will have no effect on the decay itself, and might even make the cavity more noticeable against the lighter surrounding enamel. Cavities require professional dental treatment, such as a filling, to restore the tooth.
Q6: Is it bad if a dark spot on my tooth doesn’t hurt?
A: Yes, it can still be bad even if it doesn’t hurt. Early cavities often don’t cause any pain or sensitivity because the decay hasn’t yet reached the inner, more sensitive layers of the tooth (dentin and pulp). By the time you feel pain, the cavity is usually more advanced and might require more extensive treatment. Therefore, any dark spot on a tooth, regardless of whether it causes discomfort, should be evaluated by a dentist as soon as possible.
Conclusion
The appearance of a dark spot on your tooth can certainly be alarming, prompting the immediate question: Are dark spots on teeth cavities? As we’ve explored, the answer isn’t always a straightforward “yes.” While some dark spots are indeed indicators of tooth decay, many others are harmless stains caused by diet, lifestyle, or other non-carious factors. Understanding the potential causes, from surface stains to intrinsic discoloration and actual cavities, is the first step toward addressing the issue effectively.
The most crucial takeaway is this: never self-diagnose when it comes to your dental health. Only a qualified dental professional can accurately determine the nature of a dark spot on your tooth using a combination of visual examination, dental tools, and X-rays. Early detection, whether it’s a minor stain that can be polished away or a small cavity requiring a simple filling, can save you from more extensive and costly treatments down the line.
Maintain diligent oral hygiene with regular brushing, flossing, and the use of fluoride products. Be mindful of your diet, limiting staining and sugary foods. Most importantly, schedule and keep your routine dental check-ups and cleanings. These proactive measures are your best defense against both unsightly dark spots and the progression of cavities, ensuring your smile remains healthy, bright, and confident for years to come.
