Understanding the various causes behind these visual disturbances is crucial for peace of mind and appropriate action. From the common “floaters” that drift harmlessly across your sight to more complex retinal issues, we’ll delve into the science, symptoms, and necessary steps to take. Whether you’ve just started noticing a new spot or have been living with one for a while, this article will equip you with essential knowledge, practical advice, and a clear understanding of when it’s time to consult an eye care professional. Let’s shed some light on the shadows within your vision and empower you to take charge of your eye health.
Understanding the Dark Spot On Retina: What Is It?
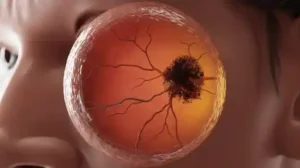
When we talk about a dark spot on retina, we’re referring to a visual phenomenon where a persistent shadow, blur, or distinct dark area appears in your field of vision, often perceived as being within the eye itself rather than an external object. The retina is the light-sensitive tissue at the back of the eye that converts light into electrical signals, which are then sent to the brain. Any obstruction or abnormality affecting how light hits or is processed by the retina can manifest as a dark spot.
It’s important to distinguish between different types of visual disturbances that people might describe as a “dark spot.” These can range from fleeting sensations to more permanent fixtures:
- Floaters: These are arguably the most common cause of perceived dark spots. They appear as small specks, squiggly lines, or cobweb-like shapes that drift across your vision, especially when looking at a bright background. Floaters are typically caused by tiny pieces of debris within the vitreous humor – the gel-like substance that fills the eye. As we age, the vitreous can liquefy and shrink, causing collagen fibers to clump together and cast shadows on the retina.
- Pigmented Lesions: These are actual dark areas on the retina itself, often identified during a dilated eye exam. They can be benign, such as choroidal nevi (freckles of the eye), or, in rare cases, indicate more serious conditions like choroidal melanoma.
- Retinal Hemorrhages: Bleeding within the retina or vitreous can cause dark spots or cloudiness in vision. This can be due to various underlying conditions, including diabetic retinopathy, high blood pressure, or retinal tears.
- Retinal Detachment or Tears: A sudden increase in floaters, flashes of light, and a “curtain” or “shadow” moving across your field of vision can indicate a serious retinal tear or detachment, which requires immediate medical attention.
- Macular Degeneration: While primarily causing blurred central vision or distortion, certain forms or stages of age-related macular degeneration (AMD) can sometimes present with scotomas (blind spots) that might be perceived as dark areas.
- Other Conditions: Inflammation (uveitis), infections, or even migraines can sometimes cause temporary visual disturbances that include dark spots.
Understanding that a dark spot on retina isn’t a single condition but rather a symptom of various underlying issues is the first step toward effective management and treatment.
Common Causes of Dark Spots and Shadows in Vision
Delving deeper into the origins of these visual anomalies helps us better understand their nature. Here are some of the most frequent causes:
- Posterior Vitreous Detachment (PVD): As mentioned, this is a very common age-related condition. The vitreous gel pulls away from the retina. While usually benign, it can sometimes pull too hard, causing a retinal tear. The sudden onset of new, numerous floaters and flashes of light are characteristic symptoms.
- Age-Related Changes: Beyond PVD, the natural aging process can lead to subtle changes in the eye’s structure, increasing the likelihood of perceiving floaters or other minor visual imperfections.
- Nevi (Freckles of the Eye): Just like skin, the choroid (a layer of blood vessels behind the retina) can develop pigmented spots called nevi. Most are benign and never cause problems, but ophthalmologists monitor them for any changes, as a very small percentage can turn malignant.
- Myopia (Nearsightedness): Highly myopic individuals are more prone to developing floaters and experiencing PVD at a younger age due to the elongated shape of their eyeballs and associated vitreous changes.
- Eye Trauma or Surgery: Any injury to the eye or certain eye surgeries can sometimes lead to the development of new floaters or other visual disturbances.
- Diabetic Retinopathy: For individuals with diabetes, high blood sugar levels can damage the blood vessels in the retina. This can lead to bleeding (hemorrhages) or the growth of abnormal blood vessels, which can cause dark spots, blurred vision, or even blindness if left untreated.
- Retinal Migraine (Ocular Migraine): These are temporary visual disturbances, often described as shimmering or zigzagging lines, blind spots, or dark areas, that can occur with or without a headache. They typically resolve within 30 minutes.
When to Seek Professional Medical Advice
While many instances of a dark spot on retina are harmless, some situations warrant immediate medical attention. It’s crucial to understand the red flags that indicate a potentially serious eye condition:
- Sudden Onset of New Floaters: If you suddenly notice a significant increase in the number of floaters, especially if accompanied by flashes of light, this could be a sign of a retinal tear or detachment.
- Flashes of Light: Seeing sudden, brief flashes of light in your peripheral vision is a strong indicator of retinal traction (the vitreous pulling on the retina) and requires urgent evaluation.
- A “Curtain” or “Shadow” in Your Vision: This is a classic symptom of retinal detachment, where a part of your visual field is obscured by a dark, expanding shadow. This is an ophthalmic emergency.
- Loss of Peripheral Vision: Any sudden or progressive loss of side vision should be investigated.
- Pain or Redness in the Eye: While not typically associated with simple floaters, pain combined with new visual disturbances could suggest inflammation or infection.
- Spots After Trauma: If you experience new dark spots or visual changes after a blow to the eye or head, seek medical attention immediately.
- Sudden Vision Loss: Any sudden, significant decrease in vision, even if temporary, is a medical emergency.
If you experience any of these symptoms, do not wait. Contact an ophthalmologist or visit an emergency room immediately. Early diagnosis and treatment can often prevent permanent vision loss.
Diagnosis and Treatment Options for Retinal Spots
When you visit an eye care professional for a dark spot on retina, they will perform a comprehensive eye exam. This typically includes:
- Visual Acuity Test: To check your sharpness of vision.
- Pupil Dilation: Eye drops are used to widen your pupils, allowing the doctor a clear view of the retina and optic nerve.
- Slit-Lamp Examination: A microscope with a bright light used to examine the front and back of your eye.
- Ophthalmoscopy: Using a specialized lens to directly examine the retina, looking for tears, detachments, hemorrhages, nevi, or other abnormalities.
- Optical Coherence Tomography (OCT): A non-invasive imaging test that uses light waves to take cross-section pictures of your retina, providing detailed views of its layers.
- Fundus Photography: Taking photographs of the retina to document its current state, useful for monitoring changes over time, especially for pigmented lesions.
Treatment Approaches:
Treatment for a dark spot on the retina depends entirely on its underlying cause:
- Benign Floaters: Most floaters do not require treatment. If they are particularly bothersome and interfere with daily activities, a vitrectomy (surgical removal of the vitreous) can be performed, but this is usually reserved for severe cases due to potential risks. Laser vitreolysis, which uses a laser to break up large floaters, is another option, though its effectiveness and safety are still debated.
- Retinal Tears: If a retinal tear is detected before it progresses to a detachment, it can often be treated with laser photocoagulation or cryopexy (freezing). These procedures create scars that seal the retina to the underlying tissue, preventing fluid from leaking and causing detachment.
- Retinal Detachment: This is a surgical emergency. Procedures like scleral buckle, vitrectomy, or pneumatic retinopexy are used to reattach the retina. The success rate is high, especially when treated promptly.
- Diabetic Retinopathy: Treatment may involve laser photocoagulation to seal leaking blood vessels or reduce abnormal vessel growth, injections of anti-VEGF medications, or vitrectomy for severe bleeding or tractional detachments.
- Choroidal Nevi: These are typically monitored with regular dilated eye exams and fundus photography. If growth or suspicious changes are observed, further imaging or biopsy may be necessary to rule out melanoma.
- Other Conditions: Inflammation, infections, or other systemic diseases causing retinal spots will be treated according to their specific diagnosis, often involving medications like steroids or antibiotics.
It’s clear that while a dark spot on retina can be a simple age-related change, it can also be a harbinger of more serious conditions. Regular eye exams are paramount, especially as you age or if you have risk factors like diabetes or high myopia.
Recommended Products for General Eye Health
While specific “dark spots on the retina” often require medical intervention, maintaining overall eye health can be a proactive step towards supporting your vision. The following products are not intended to treat or cure existing retinal conditions or dark spots, but rather to support general eye wellness. Always consult your eye care professional before starting any new supplement regimen.
Nordic Naturals Ultimate Omega
High-quality Omega-3 fatty acids (EPA and DHA) are essential for maintaining healthy vision and retinal function. This supplement supports overall eye health and can help with dry eyes.
Nature’s Way Lutein & Zeaxanthin
These powerful antioxidants are naturally found in the macula of the eye. Supplementing with Lutein and Zeaxanthin can help filter harmful blue light and protect against oxidative stress, supporting macular health.
Blue Light Blocking Glasses
While not directly treating retinal issues, reducing exposure to blue light from digital screens can help alleviate eye strain and fatigue, contributing to overall eye comfort and potentially reducing long-term stress on retinal cells.
Frequently Asked Questions About Dark Spots On Retina
Q1: What exactly is a dark spot on the retina?
A dark spot on retina refers to a visual disturbance perceived as a shadow, speck, or distinct dark area in one’s field of vision. It’s often caused by something casting a shadow on the retina, such as vitreous floaters, or it can be an actual lesion or abnormality on the retinal tissue itself, like a hemorrhage or a pigmented nevus. The specific nature of the dark spot is determined through a comprehensive eye examination.
Q2: Are all dark spots on the retina serious?
No, not all dark spots are serious. Many are benign vitreous floaters, which are common and harmless. However, some dark spots can indicate serious conditions like retinal tears, retinal detachment, bleeding, or even tumors. It’s crucial to consult an ophthalmologist if you experience new, sudden, or worsening dark spots, especially if accompanied by flashes of light, a “curtain” in your vision, or sudden vision loss.
Q3: How are dark spots on the retina diagnosed?
Diagnosis involves a comprehensive dilated eye exam performed by an ophthalmologist. This allows the doctor to thoroughly examine the retina, vitreous, and other structures of the eye. Tools like a slit lamp, ophthalmoscope, and potentially advanced imaging such as Optical Coherence Tomography (OCT) or fundus photography, are used to identify the cause and assess the severity of the dark spot.
Q4: Can dark spots on the retina be treated?
Treatment for a dark spot on retina depends entirely on its underlying cause. Benign floaters usually don’t require treatment. However, if the dark spot is due to a retinal tear, detachment, or hemorrhage, medical procedures like laser surgery, cryopexy, or vitrectomy may be necessary. If it’s related to an underlying condition like diabetes, managing the systemic disease is also key.
Q5: What can I do to prevent dark spots on the retina?
While many causes of dark spots, such as age-related floaters or nevi, aren’t preventable, you can take steps to maintain overall eye health:
- Regular comprehensive eye exams, especially if you have risk factors like diabetes or high myopia.
- Protect your eyes from injury with appropriate eyewear.
- Manage underlying health conditions like diabetes and high blood pressure.
- Maintain a healthy diet rich in eye-supporting nutrients (e.g., Omega-3s, Lutein, Zeaxanthin).
- Avoid smoking.
Q6: Is a dark spot on the retina the same as a floater?
A floater is a common type of dark spot that appears to drift in your vision. It’s caused by tiny pieces of debris in the vitreous gel casting shadows on the retina. So, while a floater is a type of dark spot, not all dark spots are floaters. Other causes include actual lesions on the retina, bleeding, or even early stages of retinal detachment, which are more serious and fixed in nature.
Conclusion: Prioritizing Your Vision Health
Encountering a dark spot on retina can be unsettling, but as we’ve explored, it represents a broad spectrum of possibilities, from the completely harmless to the critically urgent. The key takeaway is that any new or changing visual symptom, particularly one involving your retina, should always be evaluated by an eye care professional. Self-diagnosis can be dangerous, as the subtle signs of a serious condition can easily be mistaken for a benign one.
Remember the crucial distinction: while common floaters are usually harmless, a sudden increase in their number, accompanied by flashes of light, or the appearance of a persistent shadow or “curtain” in your vision, warrants immediate medical attention. Regular comprehensive eye exams are your best defense, allowing for early detection and timely intervention for conditions that could otherwise lead to permanent vision loss. Be proactive about your eye health, listen to your body, and never hesitate to seek expert advice when your vision is concerned. Your eyesight is invaluable, so protect it with diligence and care.
“`
